Description
What is Brimonidine 0.33% Erythego® Gel 15g [Mirvaso Generic]
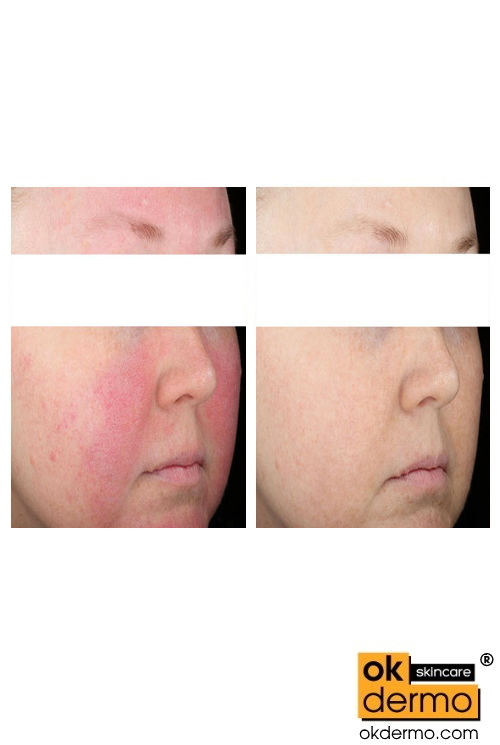
Erythego® Gel 15g is manufactured by a reputable Akumentis Healthcare Ltd company. Erythego contains the main active ingredient Brimonidine 0.33%. Erythego® Gel is an alternative/analog/generic of Mirvaso® (brimonidine) topical gel, 0.33%, is the FDA-approved treatment developed and indicated for persistent (nontransient) facial redness of rosacea. Facial redness is a common symptom of rosacea, a skin condition that affects an estimated 100 million people around the globe. Erythego® Gel is a temporary treatment for facial redness, may dramatically reduce your symptoms, but it won’t prevent or cure facial redness. Your redness will return after the effect of Erythego Gel wears off. Exposure to triggers could make your symptoms worse Avoid your triggers, even if you are using Erythego Gel as directed.
Erythego Brimonidine topical gel, 0.33% is an alpha-adrenergic agonist indicated for the topical treatment of persistent (nontransient) facial erythema of rosacea in adults 18 years of age or older.
Fast results that last up to 12 hours. Get ready for real redness relief: Erythego® (brimonidine) topical gel, 0.33% has been proven to continue to give consistent results, month after month. You can order Mirvaso brimonidine alternative online OTC via the okdermo.com skincare store.
Some patients have reported a “worsening” of redness several hours after using Brimonidine topical gel. A small percentage of patients in clinical studies reported that their facial redness returned worse than it appeared before using the gel. This could be caused by a return of the redness to the same level it was prior to using the gel, which can be concerning, especially after seeing “healthy” colored skin. Although this return of redness should go away with additional treatment, if you experience discomfort or have any concerns or questions about using Erythego Gel, contact your doctor.
The active ingredient – Brimonidine
Erythego Brimonidine 0.33% gel is chemically brimonidine and sympathomimetic by its mechanism of action. The topical gel is manufactured by the reputable Akumentis Healthcare Ltd Company. Erythego is a safe and effective way to treat the facial redness of rosacea and acne. Rosacea is a long-term skin problem that targets the face and causes redness, pimples, inflammation, swelling, and small superficial dilated veins. The nose, cheeks, forehead, and chin are the most affected parts. If severe may cause a red enlarged nose, a condition known as rhinophyma.
Brimonidine is indicated for the treatment of persistent facial erythema of rosacea in adults above 18 years of age. It is an alpha-adrenergic antagonist that works by narrowing the enlarged blood vessels of the face. This reduces the excessive blood flow to the face and thus decreases facial redness. Erythego topical gel by OKdermo is tough on rosacea and gentle on the skin. The gel fights redness with the powerful active ingredient, formulated with a gentle medical-grade gel base.
Erythego topical gel is professionally designed to show rapid results that last up to 12 hours. Erythego has been proven to continue to give consistent results month after month. Give this amazing formulation a try and you will be amazed by the results.
Get ready for real redness relief. With Erythego, forget about that redness, swelling, and itching on your face as this dermatologist’s recommended formulation will help you fight the symptoms of rosacea. Please note that Erythego provides temporary relief from facial redness and symptoms may return after you quit using the medication.
Use daily for best results treatment. Wash your hands before and after the application. Apply Erythego gel to the affected area of your face once daily. Use a pea-size amount for each area of the face. Spread the gel as a thin layer across the entire face, avoiding the lip and eye area.
Side effects of Brimonidine 0.33% Erythego® Gel 15g
In clinical trials, the most common adverse reactions (≥1%) included erythema, flushing, skin-burning sensation, and contact dermatitis.
Warnings/Precautions: Erythego Brimonidine 0.33% gel should be used with caution in patients with depression, cerebral or coronary insufficiency, Raynaud’s phenomenon, orthostatic hypotension, thromboangiitis obliterans, scleroderma, or Sjögren’s syndrome.
Alpha-2 adrenergic agents can lower blood pressure. Erythego Brimonidine gel should be used with caution in patients with severe or unstable or uncontrolled cardiovascular disease.
Serious adverse reactions following the accidental ingestion of Erythego Brimonidine gel by children have been reported. Keep out of reach of children. Not for oral, ophthalmic, or intravaginal use.
How to use Brimonidine 0.33% Erythego® Gel 15g, a Mirvaso Alternative
In clinical studies with Erythego Gel, the primary endpoint showed rosacea redness was reduced for up to 12 hours for 22% of study participants (versus 9% of people using a gel with no active ingredient [vehicle gel]). The secondary endpoint showed redness was visibly reduced in as little as 30 minutes for 28% of participants (versus 6% of people using the vehicle gel).
Getting the best results with Brimonidine 0.33% Erythego® Gel
What to expect from Erythego Gel. For most patients, the Erythego Gel effect is powerful. Skin that has been red for days, months, or even years may suddenly look “normal” again. But remember: Erythego Gel is not a cure for rosacea, your redness will return after the effect of the medication wears off.
Some patients have reported that their redness returned worse than it appeared before. This could be due to exposure to triggers or it may simply be a return to your natural complexion, which may be alarming after seeing yourself without the usual redness. Common triggers include spicy food; stress and anxiety; hot drinks, such as coffee and tea; alcohol, such as red wine; physical activity, such as exercise; sun exposure; extremely hot or cold environments; and certain skin-care products. Avoid your triggers, even while you are using Erythego gel.
Tell your doctor about the side effects. In clinical trials, about 10% of subjects reported worsening of redness while using the gel. In every case, this side effect was temporary and went away on its own. However, if you are concerned that you may be experiencing a side effect while using Erythego Gel, speak to your physician or dermatologist right away.
Order the Mirvaso brimonidine alternative via okdermo.com skin store and you will never be disappointed, best price and highest-quality products only. Buy Mirvaso gel alternative highest grade via okdermo skin care.
What Is Rosacea and where to buy Mirvaso generic?
Rosacea is a common vascular and inflammatory facial skin condition. People with fair skin over age 30 are more likely to get rosacea, but it can affect people of any age, from any background.
Facial redness and rosacea. The facial redness of rosacea, also called erythema (err-uh-thee-ma), is a common rosacea symptom—and may be the only symptom for some people. A 2012 Gallup survey asked 510 people with rosacea which symptoms they were currently experiencing and found that facial redness was by far the most common:
- Facial redness 87%
- Facial skin sensitivity to sun 51%
- Small, thin, red lines below the surface of the skin 42%
- Facial burning sensation 40%
- Pimples/pustules without blackheads 39%
- Eye redness and irritation 31%
- Pimples/pustules with blackheads 15%
- Enlarged nose or swollen bumps on the nose 14%
You might find that certain things set off your redness. Avoiding known triggers may help you manage your symptoms. Buy Mirvaso generic at the best price via okdermo.com.